Overview:
In this era, depression is a common disorder that affects adults and teenagers, who can quickly become victims. It is the primary cause of suicide in our society. But the best thing is that it can be handled with the proper anti-depression medications, lifestyle modifications, and psychological treatment.
Here, we’ll go through the different anti-depression medications and how you and your physician can select the one that will work great for you.
What Are Anti-Depression Medications?
Anti-depressants are drugs that treat depression, anxiety disorders, and other related problems like bipolar disorder, obsessive-compulsive disorder, post-traumatic stress disorder, etc.
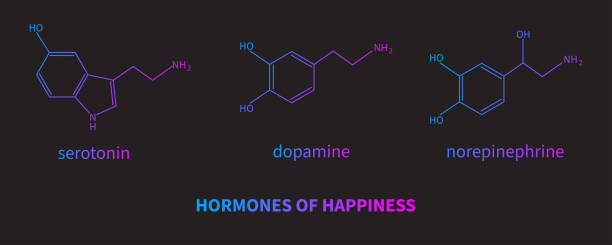
The target of these anti-depressants is brain chemicals (neurotransmitters) like dopamine, serotonin, and norepinephrine (noradrenaline) which are responsible for our mood, emotions, and anxiety. They are supposed to function by elevating the levels of certain brain chemicals.

Anti-depression medications are used to treat moderate-to-severe depression. A patient’s progress must be monitored from time to time and switched to another anti-depressant class if they do not respond to one anti-depressant class.
How Do Anti-Depression Medications Work?
The mechanism of anti-depression medications is still unknown, but many researchers say they work by elevating the levels of certain brain chemicals (neurotransmitters) like serotonin, dopamine, noradrenaline (norepinephrine), etc.
Neurotransmitters are substances in the brain that control our emotions and moods by transmitting nerve signals to receptors in the brain. The following three necessary brain chemicals are mentioned below with their functions:
- Serotonin, known as the mood stabilizer – controls appetite, digestion, sleep, blood coagulation, and mood.
- Dopamine, the reward chemical – controls sleep, lactation, learning, memory, cognition, heart, and kidney functions.
- Noradrenaline (norepinephrine) – affects attention and alertness and prepares the body for stress responses.
Over time, anti-depression medications may gradually increase the availability of one or more of these neurotransmitters. Anti-depressants often take 10 to 20 days to begin working and lessening depressive symptoms.
Best Anti-Depression Medications:
The main anti-depressant drugs are generally divided into five major classes.
Selective Serotonin Reuptake Inhibitors (SSRI)
This anti-depressant is the primary choice for treating depression and related issues. Because it has fewer adverse effects than other anti-depressants, SSRIs raise the serotonin level in the brain by preventing serotonin from reabsorption at the receptor of the receiving neuron.

The most commonly prescribed SSRIs are:
- Fluoxetine (Prozac) 20 to 60mg daily
- Escitalopram (Lexapro) 10-20mg daily
- Citalopram (Celexa) 20-40mg daily
- Sertraline (Zoloft) 50 to 100mg daily
- Paroxetine (Paxil, Pexeva) 20 to 50mg daily
- Anorexia, nausea, headaches, vertigo, and sexual dysfunction are some side effects.
Serotonin And Norepinephrine Reuptake Inhibitors (SNRIs)
Another type of anti-depressant drug is SNRI, which is identical to SSRI. The distinction between SNRI and SSRI is that SNRI raises serotonin and norepinephrine concentration, whereas SSRI (selective to serotonin) only enhances the brain’s serotonin level.

Examples of SNRIs are:
- Venlafaxine (Effexor XR) 75 to 375mg daily
- Duloxetine (Cymbalta) 60 to 20mg daily
- Desvenlafaxine (Pristiq) 50 to 400mg daily
Side effects are the same as SSRIs.
Tricyclic Antidepressants (TCAs)
The TCAs are an older class of anti-depressants. They are typically used to treat severe depression, fibromyalgia, bipolar illness, chronic pain, and sleeplessness. TCAs, however, are not the preferred option nowadays since they have hazardous side effects at larger doses. However, TCAs can still be an effective anti-depressant for those patients who fail to respond to other anti-depressants.
TCAs act like SSRIs by preventing serotonin and noradrenaline from being reuptake.
Examples include:
- Amitriptyline (Elavil) 75 to 150mg daily
- Clomipramine (Anafranil) 75 to 150mg daily
- Imipramine (Tofranil) 75 to 150mg daily
Confusion, dry mouth, hypotension, weight gain, urine retention, constipation, disorientation, sleeplessness, and sexual issues are typical adverse effects.
If a patient has prostatism, glaucoma, or cardiac problems, they should proceed with caution.
Monoamine Oxidase Inhibitors (MAOIs)
MAOIs are an older group of anti-depressants that are now seldom prescribed.
By blocking the enzyme monoamine oxidase (responsible for the metabolism of monoamines), monoamine oxidase inhibitors (MAOIs) prevent the breakdown of brain chemicals such as serotonin, noradrenaline, and dopamine in the brain. As a result, the brain chemicals in the brain increase.
Common MAOIs are:
- Emsam (selegiline) – a skin patch that may have fewer negative effects than oral MAOIs.
- Phenelzine (Nardil) 45 to 90mg daily
- Tranylcypromine (Parnate) 20 to 40mg daily
Tremors, muscle cramps, impotence, mild drowsiness, tinnitus (ear ringing or buzzing), palpitations, tachycardia, swelling of the arms or legs, paresthesia, and allergies are possible side effects.
Atypical Antidepressants
Atypical anti-depressants represent a unique class of anti-depressant drugs. If you’ve tried all the anti-depressants classes that didn’t help with your symptoms, then your physician will typically prescribe atypical anti-depressants. Each anti-depressant targets various brain chemicals, including
1- Bupropion (Wellbutrin SR, Wellbutrin XL) raises dopamine levels and norepinephrine (noradrenaline) by preventing their reuptake.
Dry mouth, nausea, weight loss, and headaches are some side effects.
2- Mirtazapine (Remeron) – is noradrenaline and specific serotoninergic anti-depressants (NaSSAs) that inhibit central presynaptic alpha-2-adrenergic receptors and increase the release of serotonin and norepinephrine (noradrenaline).
Weight gain, excessive hunger, lethargy, and sleepiness are all undesirable outcomes.
3- Trazodone (Desyrel) – is more specifically prescribed for patients with sleep issues and nightmares. Like other anti-depressants, it increases serotonin levels as well.
Side effects include fainting, fatigue, headaches, hallucinations, or irregular heartbeat (a rare side effect).
Effectiveness of Anti-Depression Medication
If an individual suffers from moderate to severe depression, anti-depressants can be helpful. But also remember that overuse or abuse can cause addiction, and addiction to anti-depressants could exacerbate the situation. Always use anti-depressants as directed by the doctor to prevent this.
The effects of these medications typically develop over time. A study found that 40% and 70% of patients experience symptom improvement between 5 and 8 weeks.
For more:
How To Get Over Depression And Anxiety Without Medication?
Summary

Depression is the most severe condition that can be treated with anti-depression medications. SSRIs and SNRIs are the first choices, but if a patient does not respond to these anti-depressants, use another instead. Each drug has side effects, and abuse can lead to addiction, so always use anti-depressants per your GP’s advice. It takes several weeks for the effects to appear.
Last, it would be best if you never stopped taking the medication without consulting the doctor who prescribed it. If you do so, it can cause withdrawal symptoms and other health-related concerns. Anti-depressants should only be stopped gradually under a doctor’s advice.